These tests each have different pros and cons (see the table below), and some of them might be better options for you than others. But the most important thing is to get screened, no matter which test you choose.
If you choose to be screened with a test other than colonoscopy, any abnormal test result should be followed up with colonoscopy.
Stool-based tests
These tests look at the stool (feces) for possible signs of colorectal cancer (or polyps). Many people find these tests easier to have than tests like colonoscopy, and they are typically done at home. But these tests need to be done more often. And if the result from one of these stool tests is positive (abnormal), you’ll still need a colonoscopy to see if you have cancer.
Fecal immunochemical test (FIT)
One way to test for colorectal cancer is to look for occult (hidden) blood in stool. The idea behind this type of test is that blood vessels in larger colorectal polyps or cancers are often fragile and easily damaged by the passage of stool. The damaged vessels usually bleed into the colon or rectum, but only rarely is there enough bleeding for blood to be seen in the stool.
The fecal immunochemical test (FIT) is also called an immunochemical fecal occult blood test (iFOBT). It tests for hidden blood in the stool. This test reacts to part of the human hemoglobin protein, which is found in red blood cells.
For this test, small amounts of stool are collected on cards (or in tubes). You can do this in the privacy of your own home. Unlike the gFOBT (see below), there are no drug or dietary restrictions before the test (as vitamins and foods do not affect the FIT), and collecting the samples may be easier. This test is also less likely to react to bleeding from other parts of the digestive tract, such as the stomach.
This test must be done every year, unlike some other tests (like the visual tests described below).
If the test results are positive (that is, if hidden blood is detected), a colonoscopy will be needed to investigate further. Although blood in the stool can be from cancers or polyps, it can also have other causes, such as ulcers, hemorrhoids, or other conditions.
 Collecting the samples: Your health care provider will give you the supplies you need for testing. Have all of your supplies ready and in one place. Supplies typically include a test kit, test cards or tubes, long brushes or other collecting devices, waste bags, and a mailing envelope. The kit will give you detailed instructions on how to collect the samples. Be sure to follow the instructions that come with your kit, as different kits might have different instructions. If you have any questions about how to use your kit, contact your health care provider’s office or clinic. Once you have collected the samples, return them as instructed in the kit.
Collecting the samples: Your health care provider will give you the supplies you need for testing. Have all of your supplies ready and in one place. Supplies typically include a test kit, test cards or tubes, long brushes or other collecting devices, waste bags, and a mailing envelope. The kit will give you detailed instructions on how to collect the samples. Be sure to follow the instructions that come with your kit, as different kits might have different instructions. If you have any questions about how to use your kit, contact your health care provider’s office or clinic. Once you have collected the samples, return them as instructed in the kit.
Guaiac-based fecal occult blood test (GFOBT)
The guaiac-based fecal occult blood test (gFOBT) detects occult (hidden) blood in the stool through a chemical reaction, in a different way than a FIT. But like the FIT, this test can’t tell if the blood is from the colon or from other parts of the digestive tract (such as the stomach).
This test must be done every year, unlike some other tests (like the visual tests described below).
This test is done with a kit that you can use in the privacy of your own home that allows you to check more than one stool sample. A FOBT done during a digital rectal exam in the doctor’s office (which only checks one stool sample) is not enough for proper screening, as it is likely to miss most colorectal cancers.
If the test results are positive (that is, if hidden blood is detected), a colonoscopy will be needed to find the reason for the bleeding. It’s not enough to simply repeat this test or follow up with tests other than a colonoscopy.
Before the test: Some foods or drugs can affect the results of this test, so you may be instructed to avoid the following before this test:
- Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil), naproxen (Aleve), or aspirin, for 7 days before testing. (They can cause bleeding, which can lead to a false-positive result.) Note: People should try to avoid taking NSAIDs for minor aches prior to the test. But if you take these medicines daily for heart problems or other conditions, don’t stop them for this test without talking to your health care provider first.
- Vitamin C in excess of 250 mg daily from either supplements or citrus fruits and juices for 3 days before testing. (This can affect the chemicals in the test and make the result negative, even if blood is present.)
- Red meats (beef, lamb, or liver) for 3 days before testing. (Components of blood in the meat may cause a positive test result.)
Some people who are given the test never do it or don’t return it because they worry that something they ate may affect the test. Even if you are concerned that something you ate may alter the test, the most important thing is to get the test done.
Collecting the samples: People having this test will get a kit with instructions from their health care provider’s office or clinic. The kit will explain how to take stool samples at home (usually samples from 3 straight bowel movements are smeared onto small squares of paper). The kit is then returned to the doctor’s office or medical lab (usually within 2 weeks) for testing.
When doing this test, have all of your supplies ready and in one place. Supplies typically include a test kit, test cards, either a brush or wooden applicator, and a mailing envelope. The kit will give you detailed instructions on how to collect the stool samples. Be sure to follow the instructions that come with your kit, as different kits might have different instructions. If you have any questions about how to use your kit, contact your health care provider’s office or clinic. Once you have collected the samples, return them as instructed in the kit.
Stool DNA test
A stool DNA test (also known as a multitargeted stool DNA test, or MT-sDNA) looks for certain abnormal sections of DNA from cancer or polyp cells. Colorectal cancer or polyp cells often have DNA mutations (changes) in certain genes. Cells with these mutations often get into the stool, where tests may be able to detect them. Cologuard®, the only test currently available, tests for both DNA changes and blood in the stool.
Collecting the samples: You’ll get a kit in the mail to use to collect your entire stool sample at home. The kit will have a sample container, a bracket for holding the container in the toilet, a bottle of liquid preservative, a tube, labels, and a shipping box. The kit has detailed instructions on how to collect the sample. Be sure to follow the instructions that come with your kit. If you have any questions about how to use your kit, contact your doctor’s office or clinic. Once you have collected the sample, return it as instructed in the kit.
This test should be done every 3 years. If the test is positive (if it finds DNA changes or blood), a colonoscopy will be needed.
Visual (structural) exams
These tests look at the structure of the inside of the colon and rectum for any abnormal areas that might be cancer or polyps. These tests can be done less often than stool-based tests, but they require more preparation ahead of time, and can have some risks not seen with stool-based tests.
Colonoscopy
For this test, the doctor looks at the entire length of the colon and rectum with a colonoscope, a flexible tube about the width of a finger with a light and small video camera on the end. It’s put in through the anus and into the rectum and colon. Special instruments can be passed through the colonoscope to biopsy (sample) or remove any suspicious-looking areas such as polyps, if needed.
Before the test: Be sure your doctor knows about any medicines you are taking (including daily aspirin, vitamins, or supplements). You might need to change how you take them before the test.
The colon and rectum must be empty and clean so your doctor can see the entire inner lining during the test. There are different ways to do this, including pills, fluids, and enemas (or combinations of these). For example, you might need to drink large amounts of a liquid laxative solution the evening before the procedure. This often results in spending a lot of time in the bathroom. Because the process of cleaning out the colon and rectum is sometimes unpleasant, it can keep some people from getting this test done. However, newer kits are available to clean out the bowel and may be better tolerated than previous ones. Your health care provider can discuss the options with you.
Your health care provider will give you specific instructions. It’s important to read them carefully a few days ahead of time, since you may need to follow a special diet for at least a day before the test and to shop for supplies and laxatives. If you’re not sure about any of the instructions, call the health care provider’s office and get your questions answered.
You will probably also be told not to eat or drink anything after a certain hour the night before your test. If you normally take prescription medicines in the mornings, talk with your doctor or nurse about how to manage them for that day.
Because a sedative is used to help keep you more comfortable during the test, you will most likely need to arrange for someone you know to take you home after the test. You might need someone to help you get into your home if you are sleepy or dizzy, so many centers that do colonoscopies will not discharge people to go home in a cab or a ridesharing service. If transportation might be a problem, talk with your health care provider about the policy at your hospital or surgery center for using one of these services. There may be other resources available for getting home, depending on the situation.
During the test: The test itself usually takes about 30 minutes, but it may take longer if one or more polyps is found and removed. Before the test starts, you’ll likely be given a sedative (into a vein) to make you feel relaxed and sleepy during the procedure. For most people, this medicine makes them unable to remember the procedure afterward. You’ll wake up after the test is over, but you might not be fully awake until later in the day.
During the test, you’ll be asked to lie on your side with your knees pulled up. A drape will cover you. Your blood pressure, heart rate, and breathing rate will be monitored during and after the test.
Your doctor might insert a gloved finger into the rectum to examine it before putting in the colonoscope. The colonoscope is lubricated so it can be inserted easily into the rectum. Once in the rectum, the colonoscope is passed all the way to the beginning of the colon, called the cecum.
If you’re awake, you may feel an urge to have a bowel movement when the colonoscope is inserted or pushed further up the colon. The doctor also puts air into the colon through the colonoscope to make it easier to see the lining of the colon and use the instruments to perform the test. To ease any discomfort, it may help to breathe deeply and slowly through your mouth.
The doctor will look at the inner walls of the colon as he or she slowly removes the colonoscope. If a small polyp is found, it may be removed and then sent to a lab to check if it has any areas that have changed into cancer. This is because some small polyps may become cancer over time.
If your doctor sees a larger polyp or tumor, or anything else abnormal, a small piece of it will be removed (biopsied) through the colonoscope. It will be checked in the lab to see if it’s cancer, a benign (non-cancerous) growth, or something else.
Possible side effects and complications: The bowel preparation before the test can be unpleasant.
The test itself might be uncomfortable, but the sedative usually helps with this, and most people feel back to normal once the effects of the sedative wear off. Because air is pumped into the colon and rectum during the test, people sometimes feel bloated, have gas pains, or have cramping for a while after the test until the air passes out.
Some people may have low blood pressure or changes in heart rhythm from the sedation during the test, but these are rarely serious.
If a polyp is removed or a biopsy is done during the colonoscopy, you might notice some blood in your stool for a day or 2 after the test. Serious bleeding is uncommon, but in rare cases, bleeding might need to be treated or can even be life-threatening.
Colonoscopy is a safe procedure, but in rare cases the colonoscope can puncture the wall of the colon or rectum. This is called a perforation. Symptoms can include severe abdominal (belly) pain, nausea, and vomiting. This can be a major (or even life-threatening) complication, because it can lead to a serious abdominal (belly) infection. The hole may need to be repaired with surgery. Ask your doctor about the risk of this complication.
CT colonography (virtual colonoscopy)
This test is an advanced type of computed tomography (CT) scan of the colon and rectum. A CT scan uses x-rays, but instead of taking one picture, like a regular x-ray, a CT scanner takes many pictures as it rotates around you while you lie on a table. A computer then combines these pictures into detailed images of the part of your body being studied.
For CT colonography, special computer programs create both 2-dimensional x-ray pictures and a 3-dimensional view of the inside of the colon and rectum, which lets the doctor look for polyps or cancer.
This test may be especially useful for some people who can’t have or don’t want to have a more invasive test such as a colonoscopy. It can be done fairly quickly, and sedation isn’t needed.
But although this test is not invasive like a colonoscopy, the same type of bowel prep is needed. A small, flexible tube is also put in the rectum for this test to fill the colon and rectum with air. And if polyps or other suspicious areas are seen on this test, a colonoscopy will still be needed to remove them or to explore them fully.
Before the test: It’s important that the colon and rectum are emptied before this test to get the best images. You’ll probably be told to follow a clear liquid diet for at least a day before the test. There are a number of ways to clean out the colon and rectum before the test. Often, the evening before the procedure, you drink large amounts of a liquid laxative solution. This often results in spending a lot of time in the bathroom. The morning of the test, sometimes more laxatives or enemas may be needed to make sure the bowels are empty. Newer kits are available to clean out the bowel and may be better tolerated than previous ones. Your doctor can discuss the options with you.
During the test: This test is done in a special room with a CT scanner. It takes about 10 minutes. You may be asked to drink a contrast solution before the test to help “tag” any stool left in the colon or rectum, which helps the doctor when looking at the test images. You’ll be asked to lie on a narrow table that’s part of the CT scanner, and will have a small, flexible tube put into your rectum. Air is pumped through the tube into the colon and rectum to expand them to provide better images. The table then slides into the CT scanner, and you’ll be asked to hold your breath for about 15 seconds while the scan is done. You’ll likely have 2 scans: one while you’re lying on your back and one while you’re on your stomach or side.
Possible side effects and complications: There are usually few side effects after this test than after colonoscopy. You may feel bloated or have cramps because of the air in the colon and rectum, but this should go away once the air passes from the body. There’s a very small risk that inflating the colon with air could injure or puncture it, but this risk is thought to be much less than with colonoscopy. Like other types of CT scans, this test also exposes you to a small amount of radiation.
Flexible sigmoidoscopy
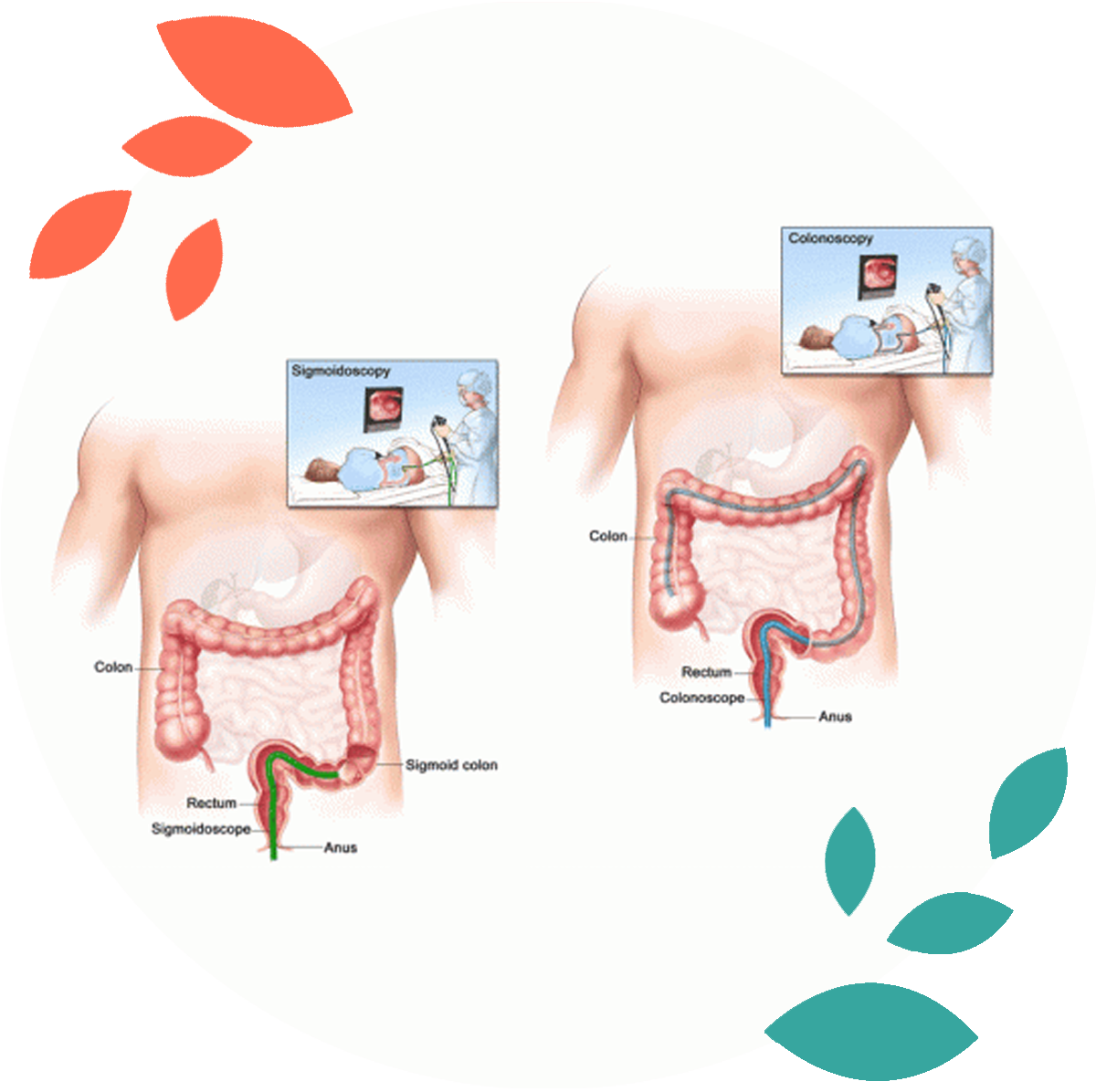
During this test, the doctor looks at part of the colon and rectum with a sigmoidoscope (a flexible, lighted tube about the thickness of a finger with a small video camera on the end). It’s put in through the anus and into the rectum and moved into the lower part of the colon. Images from the scope are seen on a video screen.
Using the sigmoidoscope, your doctor can look at the inside of the rectum and part of the colon to detect (and possibly remove) any abnormalities. The sigmoidoscope is only about 60 centimeters (about 2 feet) long, so the doctor can see the entire rectum but less than half of the colon with this procedure.
This test is not widely used as a screening test for colorectal cancer in the United States.
Before the test: Be sure your doctor knows about any medicines you take. You might need to change how you take them before the test.
Your insides must be empty and clean so your doctor can see the lining of the sigmoid colon and rectum. You will get specific instructions to follow to clean them out. You may be asked to follow a special diet (such as drinking only clear liquids) or to use enemas or strong laxatives the day before the test to clean out your colon and rectum.
During the test: A sigmoidoscopy usually takes about 10 to 20 minutes. Most people don’t need to be sedated for this test, but this might be an option you can discuss with your doctor. Sedation may make the test less uncomfortable, but you’ll need some time to recover from it and you’ll need someone with you to take you home after the test.
You’ll probably be asked to lie on a table on your left side with your knees pulled up near your chest. Before the test, your doctor may put a gloved, lubricated finger into your rectum to examine it. For the test itself, the sigmoidoscope is first lubricated to make it easier to insert into the rectum. The scope may feel cold as it’s put in. Air will be pumped into the colon and rectum through the sigmoidoscope so the doctor can see the inner lining better.
If you are not sedated during the procedure, you might feel pressure and slight cramping in your lower belly. To ease discomfort and the urge to have a bowel movement, it may help to breathe deeply and slowly through your mouth. You’ll feel better after the test once the air leaves your colon.
If any polyps are found during the test, the doctor may remove them with a small instrument passed through the scope. The polyps will be looked at in the lab. If a pre-cancerous polyp (an adenoma) or colorectal cancer is found, you’ll need to have a colonoscopy later to look for polyps or cancer in the rest of the colon.
Possible complications and side effects: This test may be uncomfortable because of the air put into the colon and rectum, but it should not be painful. Be sure to let your doctor know if you feel pain during the procedure. You might see a small amount of blood in your bowel movements for a day or 2 after the test. More serious bleeding and puncture of the colon or rectum are possible complications, but they are very uncommon.



 Collecting the samples: Your health care provider will give you the supplies you need for testing. Have all of your supplies ready and in one place. Supplies typically include a test kit, test cards or tubes, long brushes or other collecting devices, waste bags, and a mailing envelope. The kit will give you detailed instructions on how to collect the samples. Be sure to follow the instructions that come with your kit, as different kits might have different instructions. If you have any questions about how to use your kit, contact your health care provider’s office or clinic. Once you have collected the samples, return them as instructed in the kit.
Collecting the samples: Your health care provider will give you the supplies you need for testing. Have all of your supplies ready and in one place. Supplies typically include a test kit, test cards or tubes, long brushes or other collecting devices, waste bags, and a mailing envelope. The kit will give you detailed instructions on how to collect the samples. Be sure to follow the instructions that come with your kit, as different kits might have different instructions. If you have any questions about how to use your kit, contact your health care provider’s office or clinic. Once you have collected the samples, return them as instructed in the kit.